FDA Releases Final Draft AI Aesthetic Device Clinical Guidance
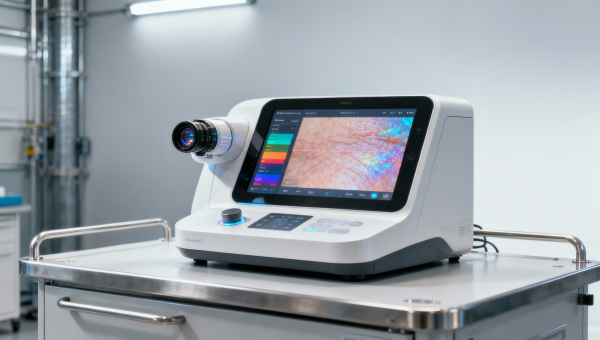
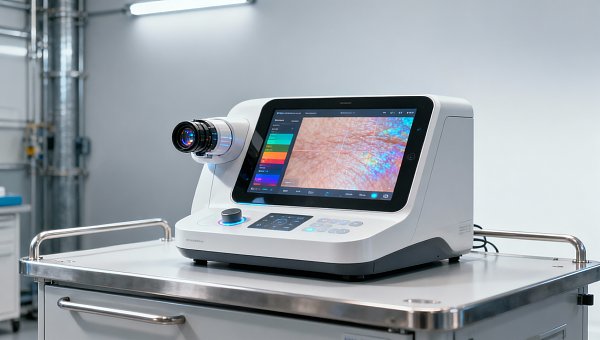
On May 13, 2026, the U.S. Food and Drug Administration (FDA) issued the final draft of its AI-Enabled Aesthetic Devices: Clinical Validation Guidance, triggering immediate attention across global aesthetic technology supply chains. The guidance introduces stringent new clinical validation requirements for AI-integrated cosmetic devices—such as AI-powered skin analyzers and adaptive radiofrequency systems—marking a pivotal shift from algorithmic transparency toward real-world clinical performance accountability. Its imminent public pre-review period, starting May 15, signals an accelerated regulatory timeline with broad implications for manufacturers, exporters, and service providers engaged in the U.S.-bound aesthetic device market.
Event Overview
The U.S. FDA published the final draft of its AI-Enabled Aesthetic Devices: Clinical Validation Guidance on May 13, 2026. It mandates that all AI-augmented aesthetic devices seeking 510(k) clearance must submit clinical data from no fewer than 500 subjects spanning diverse racial and ethnic populations—and demonstrate ≥92% concordance between AI-generated outputs and dermatologist or aesthetic physician assessments. The draft enters public pre-review on May 15, 2026, and is expected to take effect in Q4 2026.
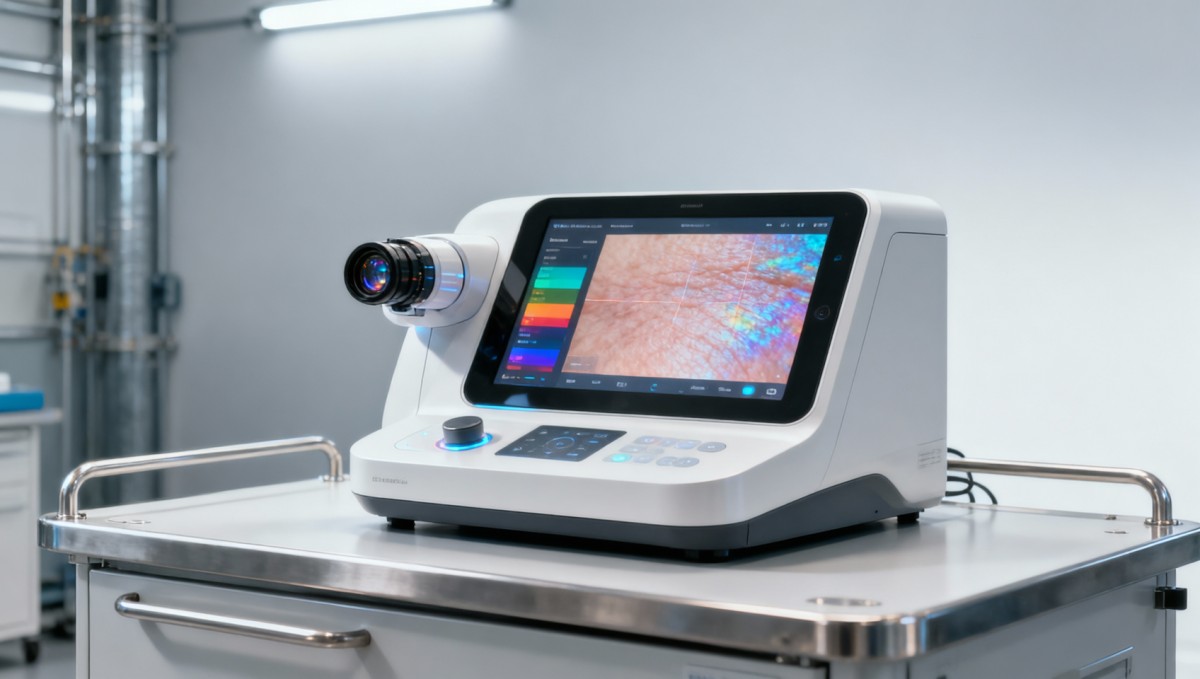
Industries Affected
Direct Exporters & Trade Enterprises
Exporters marketing AI-enabled aesthetic devices to the U.S. face direct regulatory exposure: non-compliant submissions after Q4 2026 will be rejected outright. Impact manifests in delayed market entry, increased pre-market costs (e.g., multi-center trial coordination, translation of clinical documentation), and heightened reliance on U.S.-based regulatory consultants for FDA engagement. Those lacking prior clinical trial infrastructure may see lead times extend by 9–12 months.
Raw Material & Component Suppliers
Suppliers of AI-hardware components—including edge AI chips, multispectral sensors, and calibrated thermal arrays—are indirectly affected. While not subject to clinical validation themselves, demand is shifting toward components with traceable biocompatibility certifications and documented interoperability with FDA-recognized clinical data formats (e.g., DICOM-AI extensions). Suppliers without ISO 13485 certification or clinical-grade calibration logs may lose eligibility for Tier-1 OEM tenders.
Contract Manufacturers & OEMs
OEMs—particularly China-based contract manufacturers serving global aesthetic brands—are under urgent pressure to co-develop clinical trial strategies. The 500-subject, multi-ethnic requirement cannot be fulfilled via single-site studies; thus, OEMs must now secure partnerships with clinical research organizations (CROs) operating across ≥3 geographies (e.g., U.S., Brazil, South Korea). Failure to embed clinical planning into early-stage design (e.g., defining AI output metrics aligned with clinician endpoints) risks rework post-design freeze.
Supply Chain & Regulatory Support Services
Third-party regulatory affairs firms, clinical trial management platforms, and AI validation labs are seeing surging inquiry volume—especially for services supporting cross-population data harmonization, clinician adjudication workflows, and FDA-aligned AI bias assessment protocols. Notably, demand is rising for bilingual (English–Mandarin) clinical operations managers who can bridge CRO timelines with OEM engineering cycles.
Key Considerations & Recommended Actions
Initiate Multi-Center Clinical Network Mapping Now
Given the 500-subject, multi-ethnic threshold and projected Q4 2026 enforcement, OEMs and exporters should identify and engage qualified CROs and clinical sites in at least three distinct demographic regions before Q3 2026—prior to protocol finalization—to avoid bottlenecks in IRB approvals and subject recruitment.
Reassess AI Output Definitions Against Clinician Endpoints
Per the guidance, ‘consistency ≥92%’ refers specifically to agreement on actionable clinical decisions (e.g., ‘treatment recommended’, ‘melanin index >4.2’, ‘contraindicated due to vascular lesion’)—not raw confidence scores or heatmaps. Teams must audit existing AI models to ensure outputs map directly to discrete, clinician-validated decision categories—not abstract feature vectors.
Document Algorithmic Traceability From Training Data to Clinical Output
The FDA expects traceable lineage: from source imaging datasets (with documented ethnicity, Fitzpatrick scale, lighting conditions) through preprocessing steps, model architecture choices, and final inference logic. Firms should begin compiling data provenance dossiers—including version-controlled training set inventories and clinician annotation guidelines—alongside technical files.
Editorial Perspective / Industry Observation
Observably, this guidance does not represent a de facto ban on AI aesthetic devices—but rather a deliberate recalibration of evidentiary expectations. Unlike software-as-a-medical-device (SaMD) frameworks that emphasize analytical validation, the FDA here prioritizes clinical validation: proof that AI augments, rather than replaces, human judgment in heterogeneous real-world settings. Analysis shows the 92% concordance benchmark is calibrated against inter-physician agreement rates in dermatology literature (typically 88–94%), suggesting the FDA seeks parity—not perfection. Current more critical implication lies in timing: Q4 2026 enforcement leaves minimal runway for legacy products lacking embedded clinical strategy. This makes the pre-review period (May 15 onward) less about comment submission and more about operational triage: identifying which product lines require full revalidation versus those eligible for streamlined bridging studies.
Conclusion
This guidance marks a structural inflection point—not merely a compliance update. It elevates clinical evidence from a back-end submission requirement to a front-end design constraint for AI aesthetic hardware. For the industry, the takeaway is not risk avoidance but capability acceleration: building clinical trial fluency, multi-ethnic data governance, and clinician-AI workflow integration as core competencies. Rational observation suggests the firms best positioned will be those treating FDA alignment not as a regulatory hurdle, but as a signal to invest in globally representative R&D infrastructure.
Source Attribution
U.S. FDA Center for Devices and Radiological Health (CDRH), AI-Enabled Aesthetic Devices: Clinical Validation Guidance (Draft), issued May 13, 2026. Public pre-review open May 15, 2026 via FDA Guidance Portal. Note: Final version, effective date, and potential revisions to clinical sample size thresholds or concordance metrics remain subject to change pending pre-review feedback and internal FDA review. Ongoing monitoring advised through FDA’s Docket No. FDA-2026-D-XXXXX.
Related Intelligence