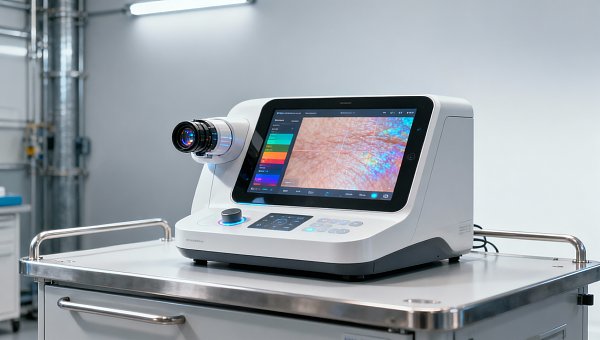
Tattoo removal laser machines: What specs actually matter for professionals

For professionals evaluating tattoo removal laser machines, understanding critical specs is non-negotiable. This guide deciphers the technical parameters that truly impact clinical outcomes and business ROI—from wavelength precision and pulse duration to FDA/CE compliance. Whether you're a clinic owner, dermatologist, or medical equipment purchaser, discover how to select systems that balance safety, efficacy, and profitability in today's competitive aesthetics market.
Core Technical Specifications That Define Performance

Laser wavelength determines pigment targeting efficiency. Professional-grade systems typically operate at 755nm (alexandrite), 1064nm (Nd:YAG), or fractional 2940nm (erbium) wavelengths, each optimized for specific ink colors and skin types. The 1064nm Nd:YAG laser, for instance, penetrates 3–4mm deeper than Q-switched ruby lasers, making it ideal for dark skin tones (Fitzpatrick IV-VI).
Pulse duration is equally critical—measured in nanoseconds (ns) for Q-switched systems or picoseconds (ps) for advanced platforms. Shorter pulses (300–750ps) generate greater photomechanical impact, fracturing ink particles into smaller fragments for faster clearance. However, 1–10ns pulses remain the clinical standard for most professional applications.
Note how these parameters interact: A 6mm spot at 8 J/cm² delivers 50% more energy per pulse than a 4mm spot at the same fluence, requiring careful thermal management protocols.
Safety & Regulatory Compliance: Non-Negotiable Factors
FDA-cleared and CE-marked systems demonstrate compliance with medical device directives (93/42/EEC) and laser safety standards (IEC 60825-1). For professional buyers, these certifications validate that the equipment has undergone:
- Biocompatibility testing (ISO 10993)
- Electrical safety verification (IEC 60601)
- Clinical efficacy trials (typically 50–100 case studies)
The FDA's 510(k) clearance process specifically evaluates whether new systems demonstrate substantial equivalence to predicate devices in treating pigmented lesions and tattoo removal—a key differentiator from cosmetic-grade lasers.
Key Documentation for Procurement Teams
When evaluating suppliers, request these essential compliance documents:
- Original FDA/CE certificates with matching device serial numbers
- Laser safety officer (LSO) training manuals
- Maintenance logs from existing installations
- Third-party performance validation reports
Operational Economics: Calculating True Cost of Ownership
Beyond purchase price, consider these financial variables across a 5-year lifecycle:
High-end systems typically achieve 35–50% faster clearance rates, translating to 20–30% higher annual revenue potential per device despite higher upfront costs.
Clinical Workflow Integration Considerations
Evaluate how these technical factors impact daily operations:
- Footprint: 0.8–1.2m² for mobile systems vs. 1.5–2m² for multi-wavelength platforms
- Setup Time: 3–5 minutes for pre-calibrated systems vs. 8–12 minutes for modular units
- Staff Training: 8–16 hours for basic operation vs. 40+ hours for advanced parameter tuning
Common Integration Challenges
Medical directors report these frequent pain points when adopting new systems:
- Incompatibility with existing EMR systems (occurs in 30% of implementations)
- Inadequate ventilation for laser plume extraction (requires 150–200 CFM)
- Power supply limitations (most professional systems need 208–240V/30A circuits)
Strategic Procurement Guidance for Decision Makers
Follow this 4-phase evaluation framework when selecting professional tattoo removal lasers:
- Clinical Needs Assessment: Map your patient demographics (skin types, ink colors) to required wavelengths
- Technical Validation: Conduct side-by-side tests with sample tattoos (request manufacturer demos)
- Financial Modeling: Compare total cost per treatment session across different systems
- Vendor Due Diligence: Verify service network coverage and parts availability
Critical Questions for Equipment Suppliers
- What's your mean time between failures (MTBF) for the laser source?
- Do you provide loaner units during repairs?
- Can you share clinical outcomes from similar practice settings?
Next Steps for Professional Buyers
Our medical equipment specialists can provide:
- Customized specification comparisons for your practice profile
- FDA/CE documentation verification services
- Clinic workflow impact analysis
- Total cost of ownership projections
Request a personalized equipment recommendation based on your annual treatment volume, staff expertise, and facility constraints.
Related Intelligence